The recent shift in global climate attributed to greenhouse effects has led to the outbreak of communicable diseases. In the previous northern winters, European and Asian states experienced a remarkably serious outbreaks of H1N1 flu, and periodic outbreaks of SARS and Avian Influenza (Bishop, Murnane, & Owen 2009, p.15). Influenza altogether is responsible for more than one million deaths.
Although vaccines for H1N1 have been available since 2009, the public response to the vaccines was not impressive. Care providers attribute this event to the previous mild nature of the H1N1 virus first-year epidemic. However, the pathogen currently seems to have transformed into a far more virulent organism, which necessitates new vaccination to control the effect of the virus. Nevertheless, the majority of the public think that vaccination is unnecessary given that the government had adopted it earlier for fear of an outbreak.
Public health staffs believe the amount of reported cases of H1N1 Flu, considerably underestimates the situation. This situation is even worse in marginal and rural areas where the public tends to undermine medical care or nursing.
The World Health Organization has developed the preferred response to outbreaks of SARS and Avian Influenza. This favored response entails involuntary quarantine and enforced segregation period from family and work of potential carriers. However, for H1N1 the favored response is voluntary quarantine and segregation, in spite of the reluctance of the Australian public to these measures recently (New South Wales Public Health Network 2009). Epidemiologists project an impending serious epidemic of the virus that will have a significant impact to the country’s economy and kill many people.
Current policy issues
Level of influenza activity and severity is monitored through the following surveillance and pointer systems (Australian Government Department of Health and Ageing 2011, p. 1):
- National Notifiable Disease Surveillance System reports of laboratory confirmed incidence;
- General Practice (GP) Sentinel Influenza-like Illness (ILI);
- Emergency Department (ED) presentations for ILI;
- ILI-based absenteeism;
- Sentinel laboratory test outcomes;
- Hospital admission, including ICU admission and deaths related with sentinel systems;
- Medical virulence in hospitalised cases as well as ICU admissions;
- Drug resistance; and
- Genetic deviation from laboratory surveillance.
The reports from the above system depict the following trend of influenza:
- Levels of ILI within the community is relatively more than previous weeks;
- All authority consistently reports higher numbers of laboratory confirmed influenza notification in summer;
- Out of 175 laboratory confirmed cases of influenza, 31 cases of H1N1 were reported. The other forms include 103 cases of influenza A and 37 cases of influenza B;
- As at April 29, 2011, the National Notifiable Disease Surveillance System (NNDSS) recorded 3,141 cases of influenza relative to 651 in2010.
However, I believe that immunization may be the best approach to control influenza pandemics. The chart below represents my projection of the impact of immunization on influenza control.
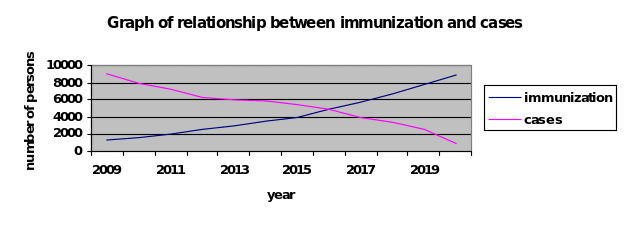
Some severe cases of H1N1 may present any underlying condition. In fact, Webb (2009) asserts that, about 30% of severe cases of the disease do not present underlying condition (p.1927). This phenomenon is the reason why, the members of the public should be keener on any flu like symptoms.
Nevertheless, most of severe cases of H1N1 are among sufferers with underlying condition. In Australia as well as in New Zealand, an unbalanced number of cases were morbidly obese, chronic lung disease, and even pregnant. Remarkably, indigenous people were also excessively probable to be admitted to ICU with the virus. Thus, there are conditions that predispose people to the disease.
Control policy
Infection control
This protocol applies for a non-hospitalised case of the disease; that is, ER, home or clinic visit. Isolation from members of the society in a unit room if possible until all the symptoms disappears. When the patient needs to move from one section of the house to another they must put on a mask. S/he should be encouraged to wash hands often and keep the respiratory hygiene principles. Cups and any other utensils used by H1N1 patient must be appropriately washed using soap and water prior to use by other individuals.
Antiviral therapy
Empiric antiviral therapy is recommended for any patient suspected to have H1N1 virus infection. Antiviral therapy with zanamivir either as monotherapy or in combination with rimantadine or amantadine must be introduced promptly following the onset of the symptoms. Optional period of treatment is five days. Recommendations for intake of antiviral can change as data about antiviral vulnerabilities become apparent. Importantly, the antiviral doses and plan suggested for the treatment of H1N1 virus infection are similar to those recommended for seasonal influenza. The antiviral therapy for verified incidence of H1N1 virus infection, physicians may administer Zanamivir or oseltamivir. Recommended period for treatment is 5 days. The same antivirals should be recommended for treatment of incidents that test positive for H1N1 flu while test negative for seasonal influenza viruses including H1 and H3 using PCR technique.
Antiviral chemoprophylaxis
Physicians recommend oseltamivir or zanamivir for antiviral chemoprophylaxis of H1N1 Flu. Period for antiviral chemoprophylaxis is averagely seven days following the last known exposure to a disease confirmed incident of H1N1 virus infection. Dosing program optional for antiviral chemoprophylaxis of H1N1 virus infection are similar too those optional for seasonal influenza.
Antiviral chemoprophylaxis is optional for the following people:
- Households close contacts at high-risk for developing complications with confirmed or suspected incident of the flu.
- Schoolchildren, who are prone to developing complications of the flu, had close interaction with a confirmed or a suspected case.
- Travellers to Mexico who are susceptible to developing complications of the influenza.
- Health care staff or public health officers who had unprotected close interaction with a sick confirmed case of H1N1 virus infection in the infectious phase of the case.
Options available to the government
The management phases
The Australian Commonwealth initiated the phases and they include the delay, contain, and protect phases. Every phase denoted different messages to the community and healthcare staff (Appuhamy, Beard, Phung, Selvey, Birrell, & Culleton 2010, p. 95).
- The objective of the delay phase was to prevent the 2009 pandemic H1N1 virus from spreading to Australia and it directed concern on the border control and correspondence with international travellers (Eastwood, Durrheim, Butler, & Jon 2010, p. 4).
- The contain phase focused on “identifying cases and tracing contacts…cases of confirmed pandemic H1N1 infection had their contacts actively managed through isolation, antiviral medication, home quarantine, and improved infection control practices to lower the spread of infection” (Eastwood, Durrheim, Butler, & Jon 2010, p. 4).
- Protect phase was inspired by the realization that H1N1 infection was less severe and the adverse effect of its workload on the provision of health care. The public health officers unit shifted its response to early detection and control of infection in persons of distinct risk group (Center for Disease Control 2010).
However, DeNoon rues that, the shift in focus from actively tracking new infections to “treating every person in Australia who presents with influenza-like illness to focusing on people in high-risk groups posed a greater risk-communication difficulty for health authorities” (2009, p.56).
On December 1, 2010, Australia shifted from the PROTECT phase to the ALERT phase of its pandemic policy. ALERT phase corresponds with a period between pandemics; that is, disease activity in terms of seasons. The important factor of the ALERT phase is keen vigilance for a novice influenza virus or functional transformation of an influenza virus currently in the body, which may raise concerns for the public health (State Government of Victoria, Australia, Department of Health 2011). Indeed, from June through August, which correspond with Southern hemisphere winter, Australia and New Zealand Intensive Care Units recorded 15 folds more H1N1 cases than in previous years.
Surveillance
Consistent surveillance for H1N1 virus has resumed, which involves clinical practitioners and laboratory notification of lab established cases and guard surveillance from common practice, hospitals and Intensive Care Units [ICUs]. The department of health advocates for the uptake of seasonal H1N1 vaccine.
Chilly conditions tend to propagate the virus since the disease is more prevalent during winter. Based on Webb (2009), the greatest demand on ICU resources in any region ensues approximately 4 to 6 weeks subsequent to the first verified winter ICU admission, and that the additional workload extends for a couple of weeks (p.1925).
ICU patients with H1N1 Flu reported a 16% mortality rate. This mortality rate corresponds with those reported in Australian hospitals in ICU patients with pandemic flu. How is pattern of prevalence within the general population for both diseases? For seasonal flu, the elderly were more vulnerable (DeNoon 2009, p. 54). On the other hand, the population segment that was more vulnerable to H1N1 influenza was the infants below age 12 months or adults between ages 25 to 64.
Policy options
There are many different policy options for control of H1N1 virus infections. The best option is Influenza vaccination.
Influenza vaccine
Influenza viruses transform often such that there is need for influenza vaccine to be updated each year. Health officers recommend every Australian resident to get an influenza vaccine every year in autumn. Protection initiates approximately two weeks after vaccination and will last for a year (Slovic, Finucane, Peters, & MacGregor 2004, p. 317). There are diverse brands of influenza vaccine although they all defend against similar strain of influenza every year.
The vaccine comprise of an injection of killed influenza virus fragments, trace amount of an antibiotic, salt water, and preservative. Scientists grow the influenza viruses in embryonic chicken eggs.
Infants and children aged between six months to 10 years of age getting influenza vaccine for the first time need two doses at minimum at one-month interval. Children below age three years receive a lesser dose of the vaccine (Stevenson, Barrios, Cordell, Delozier, Gorman, Koenig 2009, p.258). Who should get an influenza vaccine?
The National Immunisation Program Schedule facilitates this process free of charge for all people including:
- Every person aged 65 years and above
- Expectant mothers
- Aboriginal and Torres Strait Islander residents aged 15 years and above.
- All persons aged from six months and above with clinical conditions that pose them to risks of developing complications from influenza
- People in nursing homes and long-term care institution
In addition, the vaccine is strongly recommended for though may not be free of charge for:
- personnel, volunteers and regular visitors to a hospital, nursing home or long-term care facility
- an individual residing or caring for a person who has a chronic disease or is aged
- Persons offering essential services
- Employees in other industries
- Employees in poultry industry
- Travellers visiting a region of the world where influenza is prevalent or travelling in a group
Noteworthy, a person can purchase an influenza vaccine after prescription by a doctor.
Good hygiene
- Good hygiene practice such as covering one’s nose and mouth using a tissue when coughing or sneezing contribute in controlling the spread of the virus.
- Discard the tissue in a plastic-lined garbage bin after use.
- Wash hands regularly using soap and water, particularly after a cough or sneeze. Alcohol-based cleaners are preferred.
- Restrain from touching your mouth, nose, and eyes since germs propagate in that manner.
If you feel unwell
- A person should not report to work or school when s/he presents flu-like symptoms (Sandman 2009, p.323).
- A person is recommended to seek medical advice when s/he presents flu-like symptoms.
Support for recommended policy
The most effective policy for controlling the H1N1 virus breakout is immunization through an influenza vaccine. This vaccine provides all the vaccinated individuals with a one-year protection from the H1N1 virus (Hagan, Maguire, & Bopping 2008, p. 39). The influenza vaccine guarantees protection from the flu even in conditions that provides a high risk for influenza complications.
In addition, immunization helps to reduce the number of cases thereby reducing the workload on the ICU resources. This in turn helps to reduce the cost of healthcare delivery. With immunization, the virus does not get the opportunity to transform to another strain.
Policy implementation
The Australian government should ensure that all people residing or visiting Australia must get vaccine against H1N1 virus. Therefore, the government should establish influenza vaccination at the airport and border points to ensure that all persons moving into or out of Australia are immunized against the virus (Murphy 2009, p. 53).
In addition, the government should also provide vaccination services in all educational institution. The government should develop legislation requiring all organizations to vaccinate all their employees (World Health Organization 2009). In fact, it should include influenza vaccine as a requirement in medical check up process.
The government should establish a health care facility for handling strictly H1N1 only, and develop policies to keep the patients and their attendants quarantined, and isolation. Australian government should also consider enacting laws prohibiting public to visit health care facilities for H1N1 patients.
Conclusion
The public plays a significant role in determining whether a certain policy yields desired outcomes. The degree to which the community complies with the developed policy depends on their knowledge on that issue. Thus, for the public to comply with a policy, they must first be enlightened about the issue for which the policy was developed.
References
Appuhamy, R.D., Beard, F.H., Phung, H.N., Selvey, C.E., Birrell, F.A., & Culleton, T.H., 2010. The changing phases of pandemic (H1N1) 2009 in Queensland: an overview of public health actions and epidemiology. Med J 192, pp. 94–97.
Australian Government Department of Health and Ageing. 2011. Australian influenza Surveillance report: No. 3, 2011. Department of Health and Ageing.
Bishop, J.F., Murnane, M.P., & Owen, R., 2009. Pandemic influenza A (H1N1) virus. New Eng J Med, 23 (6), pp. 11-16.
Center for Disease Control, 2010. Department of Health and Human Services. Web.
DeNoon, D.J., 2009. Swine Flu May Stress ICUs This Winter. MedicineNet, Inc.
Eastwood, K., Durrheim, D.N., Butler, M., & Jon, A., 2010. Respond to pandemic (H1N1) 2009, Australia. Journal of emerging infectious diseases, 16(8), pp 50-55.
Hagan, P., Maguire, B., & Bopping, D., 2008. Public behavior during a pandemic. Australian. Journal of Emergency Management, 23 (6), pp. 35–40
Murphy, C., 2009. NHS Direct: struggling with swine flu. Web.
New South Wales Public Health Network, 2009. Progression and impact of the First winter wave of the 2009 pandemic H1N1 influenza in New South Wales, Australia. Euro Surveill. Web.
Sandman, P.M., 2009. Pandemics: Good hygiene is not enough. Nature, 45(9), pp. 322–3.
Slovic, P., Finucane, M.L., Peters, E., & MacGregor, D.G., 2004. Risk as analysis and risk as feelings: some thoughts about affect, reason, risk, and rationality. Risk Anal, 24, pp. 311–22.
State Government of Victoria, Australia, Department of health, 2011. H1N1 Influenza 09 (Human Swine Flu). Web.
Stevenson, E., Barrios, L., Cordell, R., Delozier, D., Gorman, S., Koenig, L.J., 2009. Pandemic influenza planning: addressing the needs of children. Am J Public Health, 99 (6), pp. 255–60.
Webb, R., 2009. Critical care services and 2009 H1N1 influenza in Australia and New Zealand. The New England Journal of Medicine, 361 (20), pp. 1925-30.
World Health Organization. Pandemic (H1N1) 2009 Update 61. Web.
